 Patelet Rich Plasma
Patelet Rich Plasma
How the new specialty of Regenerative Medicine repairs degenerative joint conditions and disc problems
Regenerative medicine is a new speciality in medicine that focuses on using new technologies and therapies to reverse the effects of aging on joints and discs. Regenerative medicine therapies typically include platelet rich plasma and stem cell therapy (bone marrow aspirate).
New research suggests that patelet rich plasma and stem cell therapy both accelerate the body’s own natural healing powers to treat injuries to joints, tendons, muscles and spinal discs.
What is Patelet Rich Plasma?
Platelet rich plasma, commonly referred to as PRP, is the patient’s own human blood that is spun down in a centrifuge and separated producing a concentration of platelets above the natural values commonly found in their blood. Platelet rich plasma can have as much as eight times more than the normal amount of platelets.
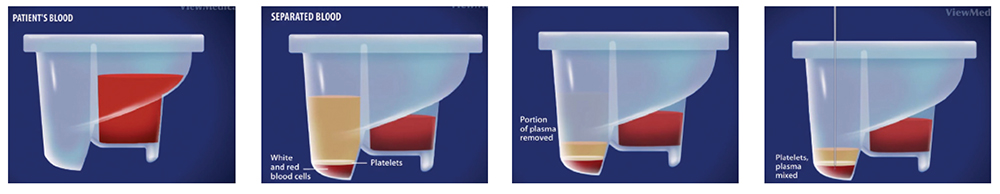
The centrifuge is used to remove red blood cells to create a plasma that has a greater concentration of growth factors than normal blood. PRP has been used in a variety of fields over the years, including plastic surgery, sports medicine and dermatology. Some professional athletes have found relief from tendonitis and overuse syndrome through PRP. The goal of PRP therapy is to enhance the body’s natural ability to repair itself to speed healing and shorten recovery time from muscle, ligament, tendon and joint injuries.
Platelets are the clotting cells within human blood that have great potential in boosting the healing of damaged muscles, tendons, and ligaments. These platelets contain natural growth hormones and proteins that tell your tissues to increase rebuilding to enhance your recovery and help stop pain symptoms.
This subsequent concentration of platelets from the patient’s own blood is then injected back into the person at the site of injury. This patelet rich plasma can then aid healing. PRP can be especially helpful for long-standing chronic injuries that have taken a long time to heal. Injecting concentrated platelets at the site of injury can accelerate the body’s own healing response.
There are some conflicting studies about the value of PRP, and which type of centrifuges may produce the optimal plasma, no studies to date have documented any adverse effects associated with PRP. So in that sense, there is no downside to the therapy. Because the injected platelets are produced from a person’s own body, there is no issue related to rejection or transmitting disease.
Who is a candidate for Patelet Rich Plasma?
Typically, the candidate for PRP has failed conservative treatment including rest, pain medication and physical therapy. However, some patients pursue PRP as an initial treatment to speed up healing. PRP can benefit patients with painful arthritis or tendonitis in the joints. PRP can also be effective for muscle injuries, meniscus and ligament injuries.
How is PRP administered?
A person undergoes PRP therapy in the physician’s office. The patient is instructed to stop all anti-inflammatory medication or steroids at least one week beforehand as these medications negatively affect platelets.
A small amount of blood (two tablespoons) are drawn from the patient’s arm. This blood sample is then placed into a centrifuge which spins the blood down so the heavier parts sinks to the bottom. Platelets and white blood cells spin out above this bottom layer and these concentrated platelets are collected and used for the injection.
Anesthesia is not necessary. A local numbing medication like lidocaine or marcaine may be used to decrease the pain at the injection site. The whole PRP treatment process typically takes less than one hour.
When do expect relief?
PRP does not provide instantaneous relief from symptoms. Growing new tissue and healling injured joints can take one to three months. But for those people who have seen their healing process stall, PRP can jumpstart the body’s own healing process.
There is great variability in the success of PRP based on the experience of the physician specializing in PRP, the type of centrifuge used, and selection of the ideal patient who can benefit from PRP.
